
14 March, 2019 - Press notes
Hospital del Mar is the first centre in Spain and one of the first in Europe to use laser technology to treat epilepsy and brain tumours safely, quickly and in a minimally invasive way. So far, three successful operations have been performed on epilepsy sufferers. In just 48 hours, they were discharged and were able to go home. The centre will operate on 10 patients each year using this pioneering technique.
Hospital del Mar is the first centre in Spain and one of the first in Europe to use laser ablation to treat cases of epilepsy and brain tumours. It is a technique that few European hospitals are capable of applying (until now only about twenty cases have been treated across the continent), and it is a result of collaboration between the Neurosurgery Service, the Epilepsy Unit, and the Radiology Service, supported by the Anaesthesiology Service. It enables the elimination of tumours and epileptic foci in a safe, quick, and minimally invasive manner, significantly reducing inpatient time after the operation.

Left to right, Dr. Jaume Capellades, Dr. Gerardo Conesa and Dr. Rodrigo Rocamora
The procedure begins by selecting patients who meet the requirements for this technique. They must have very localised lesions, whether epileptic foci or either malignant or benign tumours. In the case of epilepsy sufferers, the technique can be used to treat cases of hypothalamic hamartoma, multiple lesions, tuberous sclerosis, and deep-brain dysplasia, in addition to cavernous haemangioma, meningioma, and other pathologies.
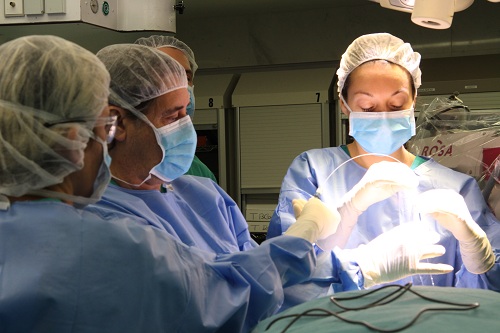
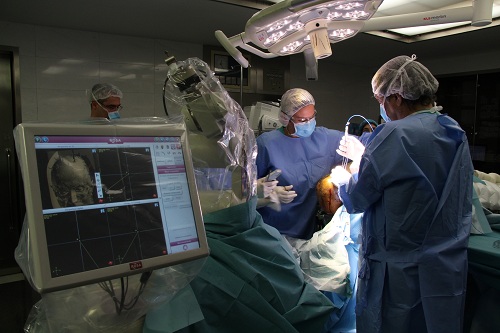
The surgery begins in the operating room, where neurosurgeons make the incisions necessary to introduce a laser probe into the patient's skull. This insertion is undertaken with the assistance of a robotic system known as ROSA®. Once the probe has been inserted, the patient is transferred to the Magnetic Resonance Unit in the Radiology Service. The anaesthetised patient is placed in a magnetic resonance tube and images are used to confirm that the point to be treated has been reached. The objective is planned and energy pulses are initiated using the VISUALASE® laser system, which burns the tissue (ablation). Dr. Jaume Capellades, head of the Neuroradiology Unit, points out that "the degree of ablation is assessed using resonance thermography maps. These allow constant monitoring of the process, and provide a high degree of precision in the induced lesion as well as, above all, safety, as the coagulation of adjacent critical structures is prevented." The pulses can be repeated as many times as deemed necessary to ensure the destruction of the damaged tissue. Working within a magnetic environment increases the complexity for the neurosurgeons and anaesthesiologists.
As Dr. Gerard Conesa, head of the Joint Neurosurgery Service at Hospital del Mar and Hospital de la Santa Creu i Sant Pau, explains, "with this technique it is possible to access lesions smaller than 3 cm in diameter in areas that are difficult to get to using conventional surgery." It should be noted that the laser allows the margins of the area to be treated to be defined more precisely and that, as it emits high energy, it burns and cauterises the tissue, thus preventing bleeding and possible haemorrhaging. In addition, "as it is a thermal technique, the procedure can be repeated as many times as necessary throughout the course of the disease", highlights Dr. Conesa.
So far, the team has performed three operations on patients, two with epilepsy and one with hamartoma, on January 24, February 20, and March 6 of this year. In all three cases, the procedure went smoothly and the patients were discharged only 48 hours after being treated. In contrast, traditional techniques mean patients have to stay in the hospital for at least a week.
Dr. Rodrigo Rocamora, head of the Epilepsy Unit at Hospital del Mar asserts that this technique "changes the paradigm of epilepsy treatment as it enables us to effectively and safely destroy lesions in locations that are complicated or dangerous for open surgery, or where that, ultimately, is not necessary." Thanks to this approach, multiple lesions can be treated in various locations, in other words, different epileptic foci can be dealt with at once if a patient is shown to have more than one. And, importantly, there are no side effects, since the areas treated "are pathological zones, with no use other than generating epileptic seizures", says Dr. Rocamora.
"This technique places no limit on the range of surgeries that can be performed on a patient", explains Dr. Conesa, who adds that "it leads the way to combining several treatments in a single operation, saving the patient from having further surgery or other types of interventions."
The Hospital del Mar team hopes to perform a dozen interventions each year on patients who meet the requirements for this type of treatment.


 This site complies with the HONcode standard for trustworthy health information:
This site complies with the HONcode standard for trustworthy health information: Parc Salut Mar
Passeig Marítim 25-29 Barcelona 08003
See location on Google maps
Phone: 93 248 30 00 · Fax: 93 248 32 54
Information request
© 2006 - 2024 Parc de Salut Mar · Legal notice and Privacy Police | Cookie Policy | Accessibility